Canada vs. U.S. Health – Report Card
Posted on | February 28, 2017 | 13 Comments

Mike Magee
In 2007, the Cambridge based National Bureau of Economic Research (NBER), self-defined as “the nation’s leading nonprofit economic research organization”, produced a singularly myopic white paper comparing the U.S. and Canadian health care systems. Noting that Canada is a “single-payer and mostly publicly-funded system” while the U.S. is a “multi-payer, heavily private system”, NBER stated that “Much of the appeal of the Canadian system is that it seems to do more for less.”
At the time of the paper, Canada was devoting about 10% of its GDP to health care versus 16% in the U.S. While spending less, Canada managed a significantly lower infant mortality rate, and higher life expectancy. The authors attempted to explain these negative findings by first noting that low birthweight is associated with high infant mortality, and then offering this analysis, “Low birthweight-a phenomenon known to be related to substance abuse and smoking-is more common in the U.S. For babies in the same birthweight range, infant mortality rates in the two countries are similar. In fact, if Canada had the same proportion of low birthweight babies as the U.S., the authors project that it would have a slightly higher infant mortality rate.”
Moving next to the troublesome issue of life expectancy, they declared, “The gap in life expectancy among young adults is mostly explained by the higher rate of mortality in the U.S. from accidents and homicides. At older ages much of the gap is due to a higher rate of heart disease-related mortality in the U.S. With such a disease, it is necessary to take with caution. While this could be related to better treatment of heart disease in Canada, factors such as the U.S.’s higher obesity rate (33 percent of U.S. women are obese, vs. 19 percent in Canada) surely play a role.”
That the NBER economists could present such arguments with a straight face well illustrates the remarkable disconnect between cause and effect, prevention and intervention, and scientific progress versus human progress in the U.S. health care system and its Medical-Industrial Complex. Eight years later Canada would boast a life expectancy of 82.2 years and an infant mortality rate of 4.9/1000 live births versus U.S. numbers of 79.3 years and 6.5/1000 live births. It should be noted as well that the per capita health care expenditure in Canada at the time was $5,292 compared to $9,403 in the U.S.
At the same time as the privately and opaquely funded NBER economists were penning their insights, actual public health leaders in Canada, after two years of thought and debate in the public square on a vision that would govern Canadian health care into the future, released its’ “ten year plan”. It included these five principles:
1)”Prevention is a priority. Canadians value their health.
2) They prefer to live a long life in good health while preventing disease or injury, rather than experiencing severe illness and the pain, suffering and loss of income that they can cause; they also want to avoid premature death.
3) Promoting good health just makes sense. While we have the means to prevent or delay many health problems, Canada’s current health system is mainly focused on diagnosis, treatment and care.
4) To create healthier populations, and to sustain our publicly funded health system, a better balance between prevention and treatment must be achieved.
5)Prevention is a hallmark of a quality health system. Internationally, health promotion and prevention are recognized as essential pieces of high-quality health systems.”
In a remarkably insightful summary, Canada’s national, provincial and territorial public health leaders declared:
“Health promotion is everyone’s business. While it is clear that health services are a determinant of health, they are just one among many. Others include:
1)environmental, social and economic conditions;
2)access to education;
3)the quality of the places where people live, learn, work and play;
4)and community resilience and capacity.
Because many of these determinants of health lie outside the reach of the health sector, many of the actions to improve health also lie outside the health sector, both within and beyond government. This means that many government departments and a wide range of people and organizations in communities and across society play a role in creating the conditions for good health that support individuals in adopting healthy lifestyles. Promoting health and preventing diseases is everyone’s business—individual Canadians, all levels of government, communities, researchers, the non-profit sector and the private sector each have a role to play.”
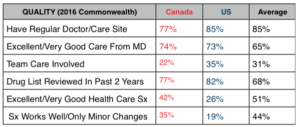
This is not to say that the Canadian health care system is perfect. Far from it. The Commonwealth Fund in 2016 compared performance of 11 developed nations on measures of quality, cost, access and communication. The charts below are derived from that survey and compare Canada, the U.S., and the average of all 11 nations.
On Quality: The U.S. compares favorably on having a regular doctor, receiving good care, and having patients drug lists reviewed. We are also a bit ahead of Canada in team care since they rely more heavily on private fee-for -service doctors. But when patients assess whether our system as a whole is optimal and whether it works well and needs only minor changes, it is clear our citizens lack confidence compared to the Canadians, and that the Canadians trail the national average.
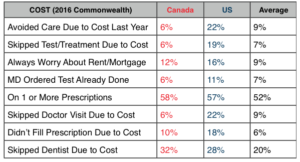
On Cost: The Canadian system does not cover dentists, eyeglasses or pharmaceuticals. If citizens want coverage for these they must purchase a private plan. Even so, the chart above clearly illustrates that U.S. citizens by significant margins feel greater financial stress than their neighbors to the north and purposefully ration their own care by avoiding necessary but expensive treatment.
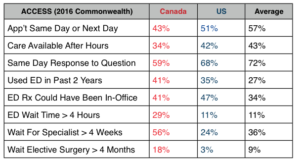
On Access: On nearly every measure, Canadians score worse on access to care than do the Americans. These are issues they have focused on for over a decade and not resolved. The waits are concentrated in the area of elective surgery and specialty referral. They have the same number of doctors per 100,000 as do Americans but have not added physician extenders and team approaches to the degree the U.S. has. Instead, they have fallen back on ED visits in the off hours, which are free, resulting in long waits after hours.
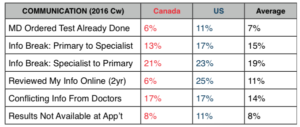
On Communications: The results are mixed. Canadians lag in their use of online medical records though the U.S. has a long way to go as well. The American system shows the signs of excessive complexity with more repeat and unnecessary tests, more breakdowns in communication between generalists and specialists, and information unavailable at the time of appointment.
By moving toward universal care, adjusting our payment incentives, inserting performance bonuses to coax quality measures and electronic medical records, President Obama was heading in the right direction. But the Republicans seem determined to roll back the clock, insert even greater complexity, and place a greater burden on vulnerable populations who’s greatest need is simplicity and clarity.
What will happen next? We’ll look at that next week.
Tags: Canadian Health Care > Canadian Health Care System > health reform > NBER > Obamacare > Paul Ryan plan
Comments
13 Responses to “Canada vs. U.S. Health – Report Card”



March 1st, 2017 @ 12:50 pm
Amazing and helpful post thanks for sharing
March 1st, 2017 @ 1:22 pm
Thanks, Haniya!
March 2nd, 2017 @ 8:16 am
Excellent and even-handed comparison. Thanks. Posted to http://www.inequalityink.org.
March 6th, 2017 @ 2:34 am
This is excellent to have. Let me say up front that I am an America. It is just like Americans to twist information that makes them look good and others look bad. Read the 1st 3 paragraphs twice. It reminds me of the accountant’s saying – “Figures don’t lie but liars sure can figure.” The U.S. should be partnering with Canada on everything.
March 6th, 2017 @ 8:22 am
Thanks, Tim. Final pieces to this contemporary exploration of what we can learn from Canada is coming soon. Mike
March 30th, 2017 @ 8:46 pm
Interesting comparison and contrast. I am a former Canadian RN (Refreshing after years off to raise kids)who has worked in several provinces in Canada (Alberta, Ontario and British Columbia) as well as several States in the US (Texas,Delaware and California). Your numbers showing that Canada actually does not reflect much more positively are eye opening because (and this is all anecdotal from mine own experiences) Canadians by and large have a positive opinion of their care and respect the “free” access afforded to them. Working in the US I never found the care lacking but attitudes were often fearful of costs and patients were shunted to different facilities based on their insurance plans.
Americans used a broader range of health care providers which Canada could adopt but Canada puts more money into the the prevention and promotion side as a way of staving off future expenditures linked to poor choices or unfortunate social/economic circumstances.Still have a long way to go, but there was a difference in the 90’s in this area.
March 31st, 2017 @ 3:05 pm
Thanks so much for your thoughtful comments. Much appreciated! Mike
August 31st, 2018 @ 5:31 pm
The analysis is interesting but the use of averages as the only measure of central tendency can hide a multitude of important distinctions.
I’d like to see medians as well. Std. Dev. is important too.
For those who haven’t been in stats class for a while — averages can be skewed by a small number of high or low values. Medians and standard deviations will show the range of the data.
I suspect that what we would find is the American system has very high and very low values on the metrics cited. If you’re rich the numbers will be very good. If you’re rich your healthcare experience will be very bad. I also suspect that the quality of healthcare in Canada is more consistent.
September 1st, 2018 @ 5:19 pm
Thanks, Matthew, for your insights and advice. I agree completely. As Wennberg noted a quarter century ago, one of the glaring deficiencies in the U.S. health care system is its level of variability. This isn’t surprising considering our income disparities, high levels of uninsured and remarkably low level of health planning and investment in the social determinants of health. Best, Mike
April 1st, 2019 @ 10:31 am
The ONLY stat that matters is all Canadians have access to healthcare. Even with the ACA all Americans do not and the reason is COST. I would say that the difference in quality of health care from one modern, western nation to another is going to be negligible… so may as well HAVE IT. America’s healthcare system has been broken for decades and anytime someone comes along with an idea to make it better it’s opposed by the right. The ACA isn’t perfect but at least it is a plan – the rights plan? They have no plan other than status quo (prior to ACA) and millions without healthcare. I dare the right to make healthcare the issue in the coming election. It will burn them.
April 3rd, 2019 @ 3:03 pm
Thanks, Randy. Well said! For historical context, see http://www.codeblue.online. Best, Mike
March 15th, 2020 @ 12:28 pm
I noticed you left out the part that the Father of Canadian Healtchare, Claude Castonguay has admitted that the Canadaian Healthcare is a failure and is in dire need of a radical overhaul.He prescribes giving the private sector a greater role so the people can excercise more freedom of choice. I kind of think that is an important part of the whole healthcare debate. I am sure he would know. Don’t you think? Go ahead Google it if you think I am lying,
March 29th, 2020 @ 9:14 am
[…] Canada vs. U.S. Health – Report Card […]