AI Assisted Measurement of The Thymus – The “Fountain of Youth?”
Posted on | May 5, 2026 | No Comments

Mike Magee
For the past eight Springs, my calendar in May has included a 90 minute lecture for the Presidents College at the University of Hartford. Both the commitment and the topic have been chosen 9 months earlier. The long lead time allows enough space to develop the in-depth research and slide deck to support topics that are often new to me. For example, this years lecture is titled “Why Immunology Could Revolutionize How We Fight Disease” and covers two centuries of discoveries culminating in the 2025 presentation of the Nobel Prize to Mary E. Brunkow, the 28th member of the American Association of Immunologists to receive the honor for her elucidation of the role of Regulatory T-cells (TREC).
The May lecture provides a baseline for a more expansive 3-session presentation of the topic in the Fall. Between Spring and Fall, the topic, its’ visuals and insights, facts and figures, expand and (hopefully) refine the narrative. So over the years, I have grown accustomed to maintaining an “eyes wide open” approach throughout the summer, for new content to appear that deserves inclusion in the Fall course.
A prime example landed on my desk two weeks ago in the form of a Nature article titled “Thymic health consequences in adults.” The article’s significance was rapidly broadcast by a range of popular science publications like Scientific American. Its March 18th headline read “This overlooked organ may be more vital for longevity than scientists realized.” It dealt with a bias I had encountered in working up the topic, that the thymus devolved over a life time, giving up its role as the creator of a repertoire of disease and cancer fighting T-cells which somehow became peripherally dispersed and almost self-guiding as independent players in our adaptive immunity system.

My final slide for next weeks lecture is both an excuse and a teaser. It acknowledges the many topics we have not covered, but also implicitly promises that our three session program in the Fall will deliver new material in these eight areas. As you can see, the last entry (#8 on my list) is “Immunosenescence (Aging).” My own notes on the topic had already referenced that the thymus shrinks with age along with its production of T-lymphocytes of varying types. I also had captured that this decline might suggest why “inflammaging” (increased levels of measurable inflammation) increase as we age, as well as the theory that a decrease in T regulatory lymphocytes might cause some blurring of the line between recognition of “self” versus “non-self,” and in so doing leave our immunologic defenses down when it came to cancer cell irradication as we aged.
The ground breaking reporting in response to the Nature article of course went much farther. Mass General publications trumpeted, “Long Dismissed in Adult Health, the Thymus May Be Critical for Longevity and Cancer Treatment,” and global outlets expanded with “Once dismissed as biologically obsolete after adolescence, the thymus is now being reclassified as a central regulator of immune aging, with new evidence linking its health to survival, cancer resistance, and how the human body ages itself.”
In their own Abstract, the authors of the Nature publication were somewhat more reserved, and yet the message is still remarkably consequential. They write, “These findings reposition the thymus as a central regulator of immune-mediated ageing and disease susceptibility in adulthood, highlighting its potential as a target for preventive and regenerative strategies to promote healthy ageing and longevity.”
Two Springs ago, at this time, I was putting the finishing touches on my Presidents College 2024 address titled “AI and Medicine.” Twenty four months later, I remain ever alert, having covered many additional breakthroughs, and the self-accelerating learnings of generative AI, and in Medicine especially. So not surprisingly what caught my eye in the case above was hardly even mentioned by reviewers who were so excited by the primary clinical findings.
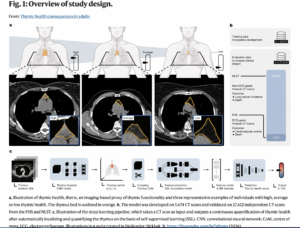
My question was, “How did they measure thymic functionality?” The short answer was, they measured it with the help of AI deep learning .
As the authors explained, “In this study, we investigated the impact of thymic functionality, here called thymic health, in adults… For quantification of thymic health, we developed a deep learning system using an independent dataset of 5,674 individuals to determine compositional radiographic characteristics of the thymus as a proxy for its functionality. The system takes a CT scan as input and provides the automatic continuous thymic health estimate as output.”
“We applied the system to prospectively collected data from a total of 27,612 individuals from two cohorts, including 2,581 participants in the FHS and 25,031 participants in the NLST (Fig. 1)… For outcome analyses, participants were categorized as low, average or high thymic health based on the bottom 25%, middle 50% and top 25% of the population.”
The capacity to demonstrate different levels of thymic functionality turned out to be groundbreaking when cross-referenced against decades long longitudinal databases. Association with cardiovascular disease and lung cancer; history of smoking, obesity, high HDL levels; disabilities, morality and mortality all reinforced that prolonged functionality of the thymus correlated with both health and longevity.
Now the authors theories could be proven. For example they stated, “As expected thymic health was higher in female than male participants and significantly declined with age.” But more than that, the authors dug deep into associations “between metabolic and thymic health,” and concluded that … these findings suggest a profound impact of actionable lifestyle choices on thymic health and may further clarify why healthy behaviour improves well-being and lifespan.”
Finally, their calculations using multiple chemical markers for inflammation, suggested that “lower thymic health was indeed associated with pro-inflammatory modifications of blood plasma protein levels, consistent with the presence of chronic inflammation. The pro-inflammatory pattern included increased levels of cytokines IL-6, IL-18 and OSM, as well as several CXCL chemokines, all of known relevance in systemic inflammatory diseases such as atherosclerosis, age-associated diseases such as arthritis, and cancer.”
In its final summary, the authors reach for the golden ring stating, “this study underscores the highly personalized nature of thymic health and emphasizes the previously unrecognized possible critical role of maintaining thymic health to preserve an agile, adaptive immune response that will accommodate long-term well-being and longevity.”
And it is understandable that they would end on such a “good news” clinical note. But we should care not to bury the lead here: Generative AI, in assisting researchers in measuring what had previously been unmeasurable, is about to reset what is “possible” in pursuing health and longevity.
Tags: aging > AI > Generative AI > immunosenescence > Medicine Research > Nature > thymus
Comments
Leave a Reply


