Canada vs. U.S. Health Care: Common Wealth
Posted on | March 8, 2017 | Comments Off on Canada vs. U.S. Health Care: Common Wealth

Mike Magee
Republicans this week demonstrated with clarity that further tinkering with our broken health care system will almost certainly add cost and undermine quality and coverage. To begin to define a way back home, we need to initially focus on two fundamental challenges.
Problem 1: Defining a National Health Care Vision
There is an actual “American Dream”. The phrase is attributed to New England social historian and writer James Truslow Adams. In 1931, he wrote The Epic of America in which he described “a dream of a social order in which each man and each woman shall be able to attain to the fullest stature of which they are innately capable, and be recognized by others for what they are, regardless of the fortuitous circumstances of birth or position.”
When Canada embarked on developing its national health care system in 1947, they identified the most knowledgeable and respected leaders they could find on the national, provincial, and territorial stages, and empowered them to create a mission and vision for Canadian health care.
Their output, reaffirmed in 2005, mirrored Adams vision. It said, in part, “As a nation, we aspire to a Canada in which every person is as healthy as they can be—physically, mentally, emotionally and spiritually.”
They defined a healthy nation as “one in which all Canadians experience the conditions that support the attainment of good health. The strategy identifies two goals: improved overall health and reduced health disparities.”
The U.S. skipped this critical strategic planning step and has been paying the price every since. Our government needs to appoint a representative body and charge them to create a consensus national vision and guiding principles for our nation’s health.
Problem 2: Disentangling the Medical Industrial Complex.
Seeing the premier academic medical institutions to the south veering off into speculative entrepreneurism, patent seeking, and fortune hunting, Canadian health leaders took the time to define the social accountability responsibilities of their medical schools. The set of principles linked the schools to the national health care system and stated in part that:
“Medical schools respond to the changing needs of the community by developing formal mechanisms to maintain awareness of these needs and advocate for them to be met”, and “Medical schools work together and in partnership with their affiliated health care organizations, the community, other professional groups, policy makers and governments to develop a shared vision of an evolving and sustainable health care system for the future.” In contrast, America’s premier academic health care systems chased the golden patent ring and research discovery laden profitability, leaving patient care and medical education in the wake.
Our “system” began as a series of self-interested professional guilds, industries, hospitals, insurers and government agencies which together formed a messy, unruly aggressive complex. For a time their conflicts with each other created some element of informal checks and balances on the system. But in the past half century, the major players in the sector infiltrated the government, and cross-fertilized each other to the point that they realized it was better and more profitable in the long run to collude behind closed doors than to fight with each other out in the open. Cooperating as an invisible united front, they now maintain control of policy, legislation and future profitability.
Piecemeal attempts by reformers have been easily repulsed. In 2008, Don Berwick acknowledged an absolute need for universal coverage and for organizational leadership. He called his leader an “integrator” who’s roles included guiding individual and family partnerships, primary care network building, population health, finances, and macro system integration. But compared to the Canadians, his faith in prevention versus carefully re-engineered high-tech intervention was qualified. His words: “Good preventive care may take years to yield returns in cost or population health.”
At around the same time Mayo Clinic’s CEO Denis Cortese, now director of Health Care Delivery and Policy at Arizona State University, endorsed “a U.S. Health Board modeled after the Federal Reserve Board… An independent board made up of providers, payers, and patients could focus on the complex decision making that must be insulated from the politics of Capitol Hill.” Yet, as we see today, politics remain front and center.
A few years earlier, two former NEJM editors offered their prescriptions for change inside the Medical-Industrial Complex. In 2004, Marcia Angell zeroed in appropriately on the pharmaceutical industry defining “how they deceive us and what to do about it”. But she appeared to deliberately leave academic medicine’s culpability unaddressed. A year later, Jerome Kassirer filled in the dots, focusing on “how medicine’s complicity with big business can endanger your health”.
He correctly concluded that “Like-minded people with ‘unique’ knowledge may have similarities of thought and come up with a uniform conclusion that is biased (or even completely wrong)”. Lending a term from the military, he highlighted “incestuous amplification” and recommended that, when filling governmental medical science advisory boards, the nation “save such ‘prizes’ for those with no financial ties, that is, to reward people who stay free of personal financial entanglements with industry.”
This is not the place, nor is there adequate space here to address how best to disentangle co-conspirators from industry, academic medicine and government. I will only say that where there is a will there’s a way – many ways.
President Obama realized, in looking for a starting point, that Governor Romney was on the right track in Massachusetts in 2006. Republican or not, the governor realized there had to be a plan; leaders had to held accountable; all citizens had to have mandated coverage because history had proven more than once they would not do so voluntarily. Channeling the spirit of our northern neighbors, Romney ally, Democratic Speaker of the House (MA), Sal DiMasi, spoke truth to power, “It was supposed to be a community of people where laws were made for the common wealth. That’s why we became a ‘commonwealth’. Nobody in Massachusetts will ever be turned away for health care”.
How should we re-organize to deliver health in America? That’s next.
Tags: Canada health care > Canadian Health > Denis Cortese > Donald Berwick > health planning > health reform > Jerome Kassirer > Marcia Angell > National Health Care > U.S. health care
Canada vs. U.S. Health Care – “You Can’t Handle The Truth!”
Posted on | March 7, 2017 | 2 Comments

Mike Magee
In the 2008 classic movie, A Few Good Men, Jack Nicholson explodes under the relentless pressure of prosecutor Tom Cruise, and yells “You can’t handle the truth!” A careful critical examiner of the US health care dilemma in 2017, in the shadow of our neighbor to the north, might easily draw the same conclusion.
As we’ve seen in the prior three segments of this series, the US health system diverged sharply from the Canadian approach in 1947, 1957, 1965 and 1984. As our costs escalated out of control, uninsured numbers rose and performance lagged, leaders expended energy defending our system as “the best health care in the world”, and defamed the Canadians and others with unsubstantiated claims that they were piggy-backing on our system to cover their own weaknesses.
In contrast to our own penchant for opaqueness, complexity and tolerance of conflict of interest, the Canadians – while far from perfect – have attempted to continuously and responsibly evolve their system and have transparently exposed their strengths and weaknesses to the light of day. As a result, Canadians support their system in far greater proportions that do the Americans.
The fact that Trump and the Republican Congress have no real plan beyond repealing Obamacare, or that the Democrats and President Obama did not manage perfection while facing constant opposition over eight years, could lead many to believe that this whole mess is just too complicated to understand let alone fix.
But the pathway out, on the surface, is pretty clear. Everyone needs to be covered to share risk. The administration and choices need to be simple and clear so that the general public can understand and participate. Elements that add cost but not value must be eliminated. And accountability must be anchored by a strategic long term plan, committed national and regional leadership, and a vision and value proposition.
What is increasingly apparent, and the truth we refuse to acknowledge, is that the problem is not the system specifically, but rather our culture and values which have been hijacked. Beginning just after WWII, but accelerating in the 1970’s and 1980’s, cross-sector leaders in energy, finance, health care and the military coordinated a deliberate attempt to seize control of power in industry, non-profits and government in pursuit of career advancement, profits, and power. These “complexes” focused on dismantling checks and balances, and managed, in a twisted dialogue among themselves, to simultaneously chase government subsidies while excoriating government intervention.
As multi-nationals expanded so did large profit-chasing, entrepreneurial “non-profits” who diligently avoided taxes while aiding and abetting the rapid expansion of poverty and income disparity. Between 1960 and 2015, “non-profits” percentage of the GDP grew three fold with 1.6 million “non-profits” now employing 10% of all American workers. As boundaries blurred, associations of associations evolved to allow coordination of government relations strategies. Attendants at their conventions were multi-sector true believers in the free-market and profits. Their cover? The claim that entrepreneurial zeal and imagineering would, through discovery, solve all of America’s problems. And those problems were growing at an alarming rate, fueled by organizations like the U.S. Chamber of Congress which spent over $1 billion lobbying in the past decade.
With President Reagan in power, enabling legislation opened the floodgates. New laws, like the 1980 Bayh-Dole Act, actively incentivized government-industry-academic non-profit collusion. In its wake, community needs faded as corporations became persons and free speech morphed into free spending. This was an opaque and deliberate hostile takeover, executed by experts with patience and near unlimited resources. Bill Moyer’s notion of “public action for public good” became a quaint euphemism for old-fashioned, out-of-touch PBS dreamers.
What felt like progress was finally revealed for what it was in the 2008 financial crisis. But this near societal collapse at the hands of free-market zealots surprisingly only tightened the embrace between the state and the private sector. The 2010 Citizen United and 2014 McCutcheon decisions solidified an American world of opaque complexes, integrated cross-sector, conflicted and cooperative power elite who continued to shift the distribution of wealth to their own kind as everyday Americans became more and more disillusioned.
So the truth we can’t handle is that, unlike Canada, we have let our highest ideals slip away from us, and we’re not quite sure how to right this ship. And yet, until we acknowledge that truth, we can’t address U.S. health care which now encompasses nearly 1/5 of our economy.
This is a nation where business and government are now largely indistinguishable from one another. This is a nation where checks and balances have melted in the face of a half century of deliberate assault creating a world absent countervailing self-correcting instincts. This is a world that for the chosen few celebrates individualism in the extreme and survival of the financially fittest, an environment where free-market ideologies routinely fail us, but then are re-subsidized and reinforced and recast by compromised insiders.
Under these conditions, we should not be surprised that the Trump administration and Congressional Republicans are now presenting health policy solutions that would increase complexity, further burden the poor and disadvantaged, and add cost at every turn.
As one commentator concluded, “Today health care in America is dominated by the medical-industrial complex…a mix of intimately interacting for-profit businesses, non-profit enterprises, and government agencies…every part of it is completely dependent on government spending and completely integrated with public-sector institutions and programs. Huge non-profit enterprises play a central role not just in the actual administration of health services but also in the generation of profits for the for-profit sector….the American health care system is both built on and reinforces an individualistic, free market ideology that simultaneous embraces government subsidization and scorns government intervention.”
That’s the truth we can’t handle. But we must. Next time – how we’ll fix it.
Tags: Canadian Health Plan > citizens united McCutcheon decision > health policy > health reform > medical-industrial complex > Obamacare > repeal Obamacare > trump > U.S. health care
Canada vs. U.S. Health – Report Card
Posted on | February 28, 2017 | 13 Comments

Mike Magee
In 2007, the Cambridge based National Bureau of Economic Research (NBER), self-defined as “the nation’s leading nonprofit economic research organization”, produced a singularly myopic white paper comparing the U.S. and Canadian health care systems. Noting that Canada is a “single-payer and mostly publicly-funded system” while the U.S. is a “multi-payer, heavily private system”, NBER stated that “Much of the appeal of the Canadian system is that it seems to do more for less.”
At the time of the paper, Canada was devoting about 10% of its GDP to health care versus 16% in the U.S. While spending less, Canada managed a significantly lower infant mortality rate, and higher life expectancy. The authors attempted to explain these negative findings by first noting that low birthweight is associated with high infant mortality, and then offering this analysis, “Low birthweight-a phenomenon known to be related to substance abuse and smoking-is more common in the U.S. For babies in the same birthweight range, infant mortality rates in the two countries are similar. In fact, if Canada had the same proportion of low birthweight babies as the U.S., the authors project that it would have a slightly higher infant mortality rate.”
Moving next to the troublesome issue of life expectancy, they declared, “The gap in life expectancy among young adults is mostly explained by the higher rate of mortality in the U.S. from accidents and homicides. At older ages much of the gap is due to a higher rate of heart disease-related mortality in the U.S. With such a disease, it is necessary to take with caution. While this could be related to better treatment of heart disease in Canada, factors such as the U.S.’s higher obesity rate (33 percent of U.S. women are obese, vs. 19 percent in Canada) surely play a role.”
That the NBER economists could present such arguments with a straight face well illustrates the remarkable disconnect between cause and effect, prevention and intervention, and scientific progress versus human progress in the U.S. health care system and its Medical-Industrial Complex. Eight years later Canada would boast a life expectancy of 82.2 years and an infant mortality rate of 4.9/1000 live births versus U.S. numbers of 79.3 years and 6.5/1000 live births. It should be noted as well that the per capita health care expenditure in Canada at the time was $5,292 compared to $9,403 in the U.S.
At the same time as the privately and opaquely funded NBER economists were penning their insights, actual public health leaders in Canada, after two years of thought and debate in the public square on a vision that would govern Canadian health care into the future, released its’ “ten year plan”. It included these five principles:
1)”Prevention is a priority. Canadians value their health.
2) They prefer to live a long life in good health while preventing disease or injury, rather than experiencing severe illness and the pain, suffering and loss of income that they can cause; they also want to avoid premature death.
3) Promoting good health just makes sense. While we have the means to prevent or delay many health problems, Canada’s current health system is mainly focused on diagnosis, treatment and care.
4) To create healthier populations, and to sustain our publicly funded health system, a better balance between prevention and treatment must be achieved.
5)Prevention is a hallmark of a quality health system. Internationally, health promotion and prevention are recognized as essential pieces of high-quality health systems.”
In a remarkably insightful summary, Canada’s national, provincial and territorial public health leaders declared:
“Health promotion is everyone’s business. While it is clear that health services are a determinant of health, they are just one among many. Others include:
1)environmental, social and economic conditions;
2)access to education;
3)the quality of the places where people live, learn, work and play;
4)and community resilience and capacity.
Because many of these determinants of health lie outside the reach of the health sector, many of the actions to improve health also lie outside the health sector, both within and beyond government. This means that many government departments and a wide range of people and organizations in communities and across society play a role in creating the conditions for good health that support individuals in adopting healthy lifestyles. Promoting health and preventing diseases is everyone’s business—individual Canadians, all levels of government, communities, researchers, the non-profit sector and the private sector each have a role to play.”
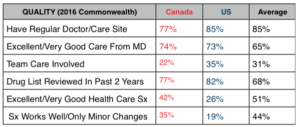
This is not to say that the Canadian health care system is perfect. Far from it. The Commonwealth Fund in 2016 compared performance of 11 developed nations on measures of quality, cost, access and communication. The charts below are derived from that survey and compare Canada, the U.S., and the average of all 11 nations.
On Quality: The U.S. compares favorably on having a regular doctor, receiving good care, and having patients drug lists reviewed. We are also a bit ahead of Canada in team care since they rely more heavily on private fee-for -service doctors. But when patients assess whether our system as a whole is optimal and whether it works well and needs only minor changes, it is clear our citizens lack confidence compared to the Canadians, and that the Canadians trail the national average.
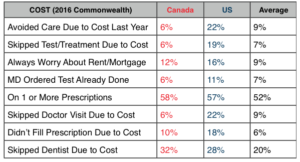
On Cost: The Canadian system does not cover dentists, eyeglasses or pharmaceuticals. If citizens want coverage for these they must purchase a private plan. Even so, the chart above clearly illustrates that U.S. citizens by significant margins feel greater financial stress than their neighbors to the north and purposefully ration their own care by avoiding necessary but expensive treatment.
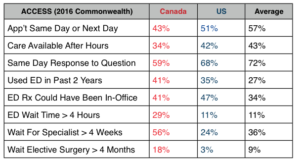
On Access: On nearly every measure, Canadians score worse on access to care than do the Americans. These are issues they have focused on for over a decade and not resolved. The waits are concentrated in the area of elective surgery and specialty referral. They have the same number of doctors per 100,000 as do Americans but have not added physician extenders and team approaches to the degree the U.S. has. Instead, they have fallen back on ED visits in the off hours, which are free, resulting in long waits after hours.
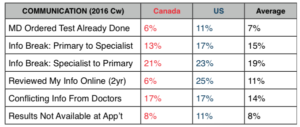
On Communications: The results are mixed. Canadians lag in their use of online medical records though the U.S. has a long way to go as well. The American system shows the signs of excessive complexity with more repeat and unnecessary tests, more breakdowns in communication between generalists and specialists, and information unavailable at the time of appointment.
By moving toward universal care, adjusting our payment incentives, inserting performance bonuses to coax quality measures and electronic medical records, President Obama was heading in the right direction. But the Republicans seem determined to roll back the clock, insert even greater complexity, and place a greater burden on vulnerable populations who’s greatest need is simplicity and clarity.
What will happen next? We’ll look at that next week.
Tags: Canadian Health Care > Canadian Health Care System > health reform > NBER > Obamacare > Paul Ryan plan
The Canadian Health Care System: The Migration Myth
Posted on | February 24, 2017 | Comments Off on The Canadian Health Care System: The Migration Myth
Mike Magee
During the Hillary Clinton health care debate of the 1990’s, our approach to health care delivery was compared to multiple other nations – including Canada. Supporters of our status quo worked hard to emphasize other nations differences and weaknesses.
The criticism of Canada, which even then was registering demonstrably better outcomes at a fraction of our cost, was twofold. First our health leaders accused the Canadians of rationing services and delaying life-saving treatments. And second, they claimed that our neighbors were able to get away with this because we were on their southern border, and Canadians in large numbers emigrated to our institutions to get access to services denied by their own niggardly system. Additionally we claimed that Canadian doctors were so dissatisfied with their system that they were routinely relocating to the U.S. to practice medicine.
These paired and interdependent false realities were presented with such certainty, and reinforced by our own medical elites so consistently, that physicians like myself bought into the propaganda without critically examining the facts. It was a full decade before these false claims were analyzed in earnest. In 2002, four health policy experts, with the support of the Canadian Medical Council, which had renamed itself the Canadian Institutes of Health Research, established unequivocally that the claims of medical migration, by either patients or their doctors, were bogus.
The Health Affairs publication, titled “Phantoms in the Snow: Canadians’ Use of Health Care Services in the United States”, didn’t mince words. Backed up with an array of facts and figures, and exhaustive documentation, the authors stated, “Results from these sources do not support the widespread perception that Canadian residents seek care extensively in the United States. Indeed, the numbers found are so small as to be barely detectible relative to the use of care by Canadians at home.”
On the Canadian side, only 90 of 18,000 citizens surveyed had used American services, and the vast majority of these were tourists seeking emergency care while traveling. Surveys of major U.S. academic centers, including those in border states reinforced the same conclusion: few if any Canadians. In the end, the authors concluded, “The numbers of true medical refugees—Canadians coming south with their own money to purchase U.S. health care—appear to be handfuls rather than hordes.” The same held true for Canadian doctors who had little to no interest in relocating.
Concurrent studies did reveal that Canadian waits for certain elective procedures and access to high tech diagnostics were longer than in the U.S. This fully transparent trade-off, made by provincial and territorial health governing bodies, was largely supported by Canadians as necessary and responsible budget management of priorities. They never hid the fact, but rather raised it in the public square. And recent corrective measures have not been entirely successful. (Message: Canada’s health care system does continue to have its own challenges.)
Absent proof of an escape valve migration south, U.S. detractors continued to wave the bloody flag of rationing, even as studies of our own system revealed that our population is more likely than citizens from other developed nations to put off needed treatment because they can’t afford it – de-facto financial self-rationing if you will.
In 2003, the U.S. under President George W. Bush continued to struggle to control health care costs. The nation’s response, with the opaque support of PhARMA, the AMA and AAMC, and the hospital and insurance industries, was to approve Medicare Part D’s non-negotiable coverage of pharmaceuticals for seniors at prices roughly 150% of the cost of Canadian counterparts.
Gallop polls at the time found that 57% of Canadians were “very” or “somewhat” satisfied with their health care system compared to 25% of Americans. 44% of our citizens were “very dissatisfied” while only 17% of Canadians felt the same. Part of the reason for relative calm up north was that their system was continuing to evolve in the full light of day. What were they up to?
In 2004, Canada’s Prime Minister and the provincial and territorial leaders announced “A 10-Year Plan to Strengthen Health Care”. Their opening statement? “As a nation, we aspire to a Canada in which every person is as healthy as they can be-physically, mentally, emotionally and spiritually.” Their guiding principles don’t sound like ours – no words like innovation, entrepreneurship, precision health or highly leveraged technologic wonders; no battles for ever increasing research funding by competing diseases; no academic goliaths with million dollar CEO’s overseeing patent producing enterprises as patient care takes a back seat.
What are their benchmarks and how is Canada performing compared to the US these days? More on that next week.
Tags: Canada's health care system > Canadian Health Care > health care design > patient migration from canada > US health reform
The Canadian Health Care System – Choices Made (Vs. U.S.) in 1947, 1957, 1964, 1984.
Posted on | February 15, 2017 | 4 Comments

Mike Magee
America’s attention is once again on health reform. Even as Republican governors preach caution, the Republican controlled Congress continues to vow to repeal the Affordable Care Act and turn Medicaid into block grants. The U.S. doesn’t exactly have a great track record when it comes to health policy decisions. Compared to Canada, we’ve consistently chosen “free enterprise” approaches that have been singularly disappointing in performance. Scientific progress has become unlinked from human progress. And the Medical-Industrial Complex continues to grow in size and appetite, while health outcomes and value for the dollar are hard to come by. In the next few weeks, we’ll take a look at our two countries to see what we can learn. We begin with an analysis of critical decisions at four moments in history – 1947, 1957, 1964, and 1984.
In 1947, in the wake of WW II, the Canadian Province of Saskatchewan launched the first provincial universal public hospital insurance plan. South of the border, the U.S. chose a very different path. With inducements in the tax code, and exemption from war time wage and salary controls, our government encouraged private employers to provide their workers with health insurance as part of what would become a standard benefit package.
A decade later in 1957, Canada passed the Hospital Insurance and Diagnostic Services Act which provided 50/50 cost sharing between the federal government and any of 13 provinces and territories that chose to participate in universal coverage of their respective populations. In the U.S. employer based insurance had now been extended to nearly 70% of Americans, pharmaceutical profiteers were being lined up for interrogation by Senator Kafauver’s Commission, and the AMA was mapping out its strategy to defeat “socialized medicine”.
In 1964, against the opposition of the Canadian Medical Society, Canada’s Royal Commission on Health Services, recommended and soon succeeded in launching a comprehensive and universal national health program. The program, called Medicare, covered everyone but not everything (pharmaceuticals,eyeglasses, dental care, and home care were exempted). They did however include federal planning and standards to promote and maintain optimal preventive health of all Canadians. A federal governance body was in charge of standards, but the delivery of care was strictly deligated to the provinces and territories who themselves managed and prioritized annual budgets, and designed their own governance systems.
In the U.S. at the same time, President Johnson in the wake of President Kennedy’s assassination, and with some skillful maneuvering by veteran legislator Wilbur Mills, passed our own Medicare, a universal program as well, but only for citizens over 65. It was federally funded and federally directed, having proven a few years earlier that voluntary enrollment programs controlled by individual states would fail. They also passed Medicaid, which like the Canadian program included a mix of federal and state funding, and delegation of responsibility for care delivery to the states. Standard setting was weaker than in Canada, and wide variability became immediately apparent both in the definition of who qualified, what was covered, and the level of each states financial commitment to services.
The Canadian government at the time held tightly to the principle of universality and public funding with federal and territorial governments serving as “single-payers”. This decision was grounded in the philosophy that Canada’s success ultimately depended on the health of Canadians, that this health was a human right, and that excessive administration would drive up cost and complexity, placing an undue burden on their citizens. Fee schedules were standard across geography and population, and negotiations with doctors and hospitals in each province or territory, as part of the budget setting process, allowed for prioritization and full transparency. Providers submitted bills for services. Government paid the bills. And the patient was left alone.
The U.S. chose an opposite course. With full faith in capitalism and competition, they reasoned that inclusion of private insurance companies, who were already deeply entrenched in their employer based health insurance system, would through competition with each other hold costs in check. U.S. doctors as well billed fees for services, but there were no annual budgets, highly variable rules and coverage, and remarkable complexity and variability that confused everyone. It also didn’t hold down costs, as insurers, responding to their shareholders managed to remove at their peak 25 cents on the dollar for their services.
In 1984, as part of their national commitment to continuous thoughtful evolution, the Canadian government passed the Canada Health Act which combined their hospital and medical acts and refined and reinforced their administration of the program as well as four anchoring pillars – portability, accessibility, universality and comprehensiveness. The deliberations were out in the open and fully transparent.
In 1984, with U.S. health care costs careening out of control, and an AIDS epidemic gaining steam absent government leadership, the U.S. once again placed all her cards on “private enterprise”. Four years earlier, in the waning days of a one term presidency mired in recession, President Carter had reluctantly signed the Bayh-Dole Act. The legislation released 26,000 federal patents (derived from federally funded research) for private use by industry and academic health centers. The scientific progress unleashed was undeniable, but the loss of checks and balances and the realignment of values and power within premier academic health centers uncoupled entrepreneurship and scientific progress from human progress. An unholy alliance at the center of a medical-industrial complex had been consummated.
Next Week: Canadian Health Care: Facts and Fiction.
Tags: Bayh-Dole Act > Canada Health Act > Canadian Health Care System > employer based health care
Indiana University’s Aaron Carroll Debunks US Prejudices Toward Canadian Health Care
Posted on | February 10, 2017 | Comments Off on Indiana University’s Aaron Carroll Debunks US Prejudices Toward Canadian Health Care
Source: The Atlantic
Press Here
Off-Label Prescribing – Where Lupron is the Rule, Not the Exception – and Doctors Never Have To Say They’re Sorry.
Posted on | February 8, 2017 | Comments Off on Off-Label Prescribing – Where Lupron is the Rule, Not the Exception – and Doctors Never Have To Say They’re Sorry.
Credit: U. Michigan Health Lab
Mike Magee
After a remarkably turbulent decade in the shadows of America’s Medical Industrial Complex – a span that has witnessed the creation of a manmade opioid epidemic, the treatment of thousands of 2 and 3 year old’s with Adderall, the placement of EpiPen’s out of the financial reach of Middle America after convincing most public schools that they were essential as portable defibrillators, the approval of an HHS secretary with a documented track record of insider trading reinforced by his own sponsored beneficial legislation while a Congressman – after all that, we are now poised to further liberalize the FDA in the name of “innovation”.
Unless one lives in an alternate reality where “alternate facts” prevail, there is no reason to further reward purveyors of off label marketing, physician profiled targeted sales, and sloppy prescribers. As Christina Jewett of Kaiser Health News has so well documented, this is the World of Lupron.
Lupron is the brand name for leuprorelin, an injectable blocker of gonadotropin releasing hormone. By interrupting the pulsed release of LH and FSH from the pituitary, the medication causes dramatic reductions of estradiol and testosterone. In adults, it’s most often used to treat prostate cancer and certain types of breast cancer, and sometimes is part of the therapy for endometriosis. Leuprorelin was first approved for use by the FDA for prostate cancer in 1985. Eight years later, it was approved for the treatment of precocious puberty in children, described as the onset of sexual characteristics “before age 8 in girls and before 9 in boys.” The cost for two years of treatment today can approach $40,000.
The FDA approving medical officer in 1993, Alexander Fleming, in retrospect later termed his approval “regrettable”. His regret was likely fueled by two factors. First, shortly after Lupron’s approval for the treatment of precocious puberty in 1993, doctors, with the blessing of manufacturers, began to treat children of “short stature” off-label with the drug. This is entirely legal in the U.S. The manufacturers are prohibited from marketing the product for unapproved uses, but they are allowed to provide doctors with information regarding off-label use if requested. The controlling company back then, TAP Pharmaceuticals, apparently pushed the envelop a bit too hard leading to government fines for “fraudulent pricing and marketing practices” of $875 million in 2001.
Dr. Fleming’s second regret, related to the first, was that manufacturers had systematically downplayed complications and side effects of the drug. Most notable were the omissions of significant bone disorders and fractures. Over the past decade, more than 20,000 reports of Lupron side-effects have been registered with the FDA, 900 in children under 13. In 2003, a NEJM article raised the alarm that kids on the drug were losing bone density at an alarming rate. Then in 2009, an international body including pediatric endocrinologists questioned the safety of using the puberty delaying drug to add inches to children’s stature. A 2011 study at Children’s Hospital of Los Angeles echoed the concerns about osteoporosis. Still the practice continued. How was that possible?
An industry 2010 study, published in a non-peer reviewed journal by Dr. Peter A. Lee of Penn State, reported side-effects with the drug between 1991 and 2009, but no bone issues. A subsequent independent review of the NIH clinical research repository revealed omission of bone fractures and disorders under complications. Further investigation in the Medicare Open Payments database revealed that Lupron’s now owner, AbbVie, paid Dr. Lee $157,066 from 2013 to 2015 to travel and promote Lupron to health professional groups. 2015 sales of Lupron netted $826 million for AbbVie.
For the Medical-Industrial Complex, which has systematically dismantled checks and balances, Lupron is the rule, not the exception. And too many doctors are cogs in the wheel, remarkably naive and susceptible to slick pitches and value laden inducements. Precocious puberty occurs in about 2000 American kids each year. And yet, doctors wrote 24,000 prescriptions for pediatric Lupron in 2015. America’s patients need the FDA to stand tall. Now is exactly the wrong time to go weak and wobbly on us.
Tags: adderall > christina Jewett > drug approval > FDA > Kaiser Health News > Lupron > luprorelin > opioid epidemic